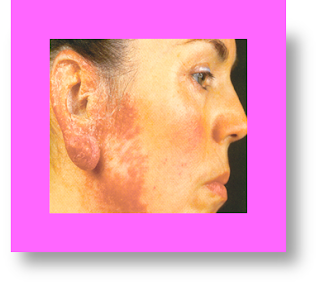
Lupus vulgaris (LV): a chronic & progressive pauci-bacillary type of cutaneous TB representing reactivated TB in subjects with moderate-high anti- TB
Lupus vulgaris (LV)
Lupus
vulgaris (LV): a chronic &
progressive pauci-bacillary type of cutaneous TB
representing reactivated TB in subjects
with moderate-high anti- TB immunity.
LV may be developed
due to direct extension of an underlying TB focus
or though lymphatic/hematogenous spread. Alternate term:
TB lupus.
Risk
factors: LV
is the most common type of cutaneous TB
in Europe
and certain zones in India. In
contrary, scrofuloderma seems
to be more observed in some tropical zones.
LV can occur in
ALL ages. It is not certain why females are 2-3
times more likely as compared to
males to be involved. LV
has also been observed in ptns with previous TB verrucosa
cutis, scrofuloderma, and rarely
as a sequela of BCG vaccination or primary inoculated TB. Despite the most commonly causing organism
is M. TB,
there’re documented cases related to M. bovis, & clinical picture is
simulating LV related
to M. TB. Subjects at risk for M. bovis LV are the resident in rural zones, contacting cattle,
or consuming infected milk products.
Clinical
presentation: clinical findings of LV
are variable. Typical plaque presentation starts as a collection of discrete, red-brown
papules with subsequent coalesce to be an indolent, asymptomatic
plaque. The plaque gradually extends peripherally to reach 0.5-10 cm with central clearance & atrophy. Lesional borders may show serpiginous or
verrucous quality. Hypertrophic, ulcerative,
& vegetative form of LV can be also be
seen. Lesions with secondary infection may show a seropurulent
discharge with crust formation. In
the West, LV often
observed on the head & neck, while
in tropical & subtropical zones, lesions are commonly seen on the lower limbs
or buttocks. Similar to other granulomatous lesions,
e.g., sarcoidosis & leprosy, diascopy (examining
the lesion with compression via a glass slide)
of non-hyperkeratotic areas of LV usually show a yellow-brown color
known as an "apple jelly".
However, it is difficult to observe with dark skin.
Dgx: LV is a paucibacillary type of cutaneous TB, & mycobacteria usually cannot be identified
by biopsy or culture. However, Dgx supported by evident clinical & histopathologic pattern
& +ve nucleic acid amplification (NAA) testing. Tuberculin testing can be also +ve.
Histopathology may show tuberculoid granuloma + discrete,
central caseation in upper dermis. Epidermis
could be atrophied or acanthotic + excessive
hyperkeratosis or pseudo-epitheliomatous
hyperplasia. Dermatoscopic testing may show well-focused, linear-branching
telangiectasia on a diffuse/localized,
structureless, yellow/orange background
+ whitish, reticular streaking.
DD: LV shares clinical findings with many
disorders. Papular lesions should be DD from colloid milia, acne,
& rosacea. Plaques may simulate deep fungal infection, Leishmania, late
syphilitic infection, discoid lupus,
tuberculoid leprosy, & psoriasis. Course: with
no ttt, lesion of LV
persists & may grow to enormous size over years. Ulceration
& destruction of tissues, e.g.,
nose, ears, & lips, could be seen > severe disfiguring. Squamous cell carcinoma may develop in long-standing disorders. Rarely, basal cell carcinoma
can be seen in long-standing LV locations.












COMMENTS