Cutaneous manifestations & Dermatologic care IN COVID-19
Cutaneous
manifestations &
Dermatologic
care IN COVID-19
A variety of cutaneous manifestations have been
reported in ptns with confirmed diagnosis or suspected severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)
disease that may include a morbilliform rash;
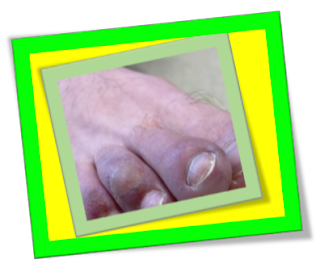
urticaria; pernio-like, acral lesions;
livedo-like, vascular lesions; & vesicular, varicella-like
eruptions. A severe multisystem inflammatory syndrome with muco-cutaneous,
systemic, lab profile, and multiple imaging
of atypical, severe Kawasaki disease has also been observed in children &
adolescent COVID-19 infection. Skin injury, mechanical/friction
dermatitis, & hand irritant
contact dermatitis owing to personal protective equipment (PPE) &
hand hygiene precautions have been observed in most of the health care stafs involved
in the care of ptns with COVID-19 infection.
The use of a barrier film or dressings at pressure points of PPE,
in addition to the frequent use of emollients after hand washing may help reducing skin damage
& irritation.
The COVID-19
pandemic has its contribution in the need to consider the aspects of dermatologic care. For example, adjustment of
the approach to im/m medications, phototherapy, skin
cancer medications, in addition to the routine clinical care. The
impact of immunosuppressive therapy (im/m)
for dermatologic lesions on risk for developing SARS-CoV-2
infection and risk for COVID-19 sequela
still uncertain. The decision to continue or to commence im/m therapy for dermatologic disease during pandemic
era should be currently individualized. Examples of important factors to
consider include the ptn's infectious state, the im/m
under consideration, and the impact of therapy cessation on the dermatologic
diseases and other co-morbidities. In view of the lack of evidence indicating
benefit of im/m withdrawal in ptns
without COVID-19, continuation of im/m agents for dermatologic disease can be
considered a safe & appropriate
option in this cohort. The option to commence a new im/m
agent should include careful consideration of potential risk & benefit of therapy. In ptns
with risk for severe COVID-19 disease,
it may be wise to defer im/m agents
in favor of other therapies.
Infection activity is a crucial indication for withdrawal
& avoidance of start of im/m agents,
and some professional institutes, including the American
Academy of Dermatology, have provided statements that recommend withdrawal
of im/m drugs for skin disease in ptns
developing COVID-19 infection. In
view of the paucity of evidence on risks & benefits of discontinuation, our decision to continue or
discontinue an im/m agent in ptns
with presumed/confirmed COVID-19 infection
may be proceeded on an individualized basis. If withdrawn, an im/m agent may be resumed with documented complete recovery form
COVID-19. The COVID-19 pandemic has contributed to prevalent
use of telemedicine for routine patients’ care. With in-person visit,
the appropriate infection control measures should be undertaken.
REFERENCES
- Freeman EE,
McMahon DE. Creating dermatology guidelines for COVID-19: The pitfalls of
applying evidence-based medicine to an emerging infectious disease. J Am
Acad Dermatol 2020; 82:e231.
- Galván
Casas C, Català A, Carretero Hernández G, et al. Classification of the
cutaneous manifestations of COVID-19: a rapid prospective nationwide
consensus study in Spain with 375 cases. Br J Dermatol 2020; 183:71.
- de Masson
A, Bouaziz JD, Sulimovic L, et al. Chilblains is a common cutaneous
finding during the COVID-19 pandemic: A retrospective nationwide study
from France. J Am Acad Dermatol 2020; 83:667.
- Freeman EE,
McMahon DE, Lipoff JB, et al. Pernio-like skin lesions associated with
COVID-19: A case series of 318 patients from 8 countries. J Am Acad
Dermatol 2020; 83:486.
- Daneshgaran
G, Dubin DP, Gould DJ. Cutaneous Manifestations of COVID-19: An
Evidence-Based Review. Am J Clin Dermatol 2020; 21:627.
- Guan WJ, Ni
ZY, Hu Y, et al. Clinical Characteristics of Coronavirus Disease 2019 in
China. N Engl J Med 2020; 382:1708.
- Recalcati
S. Cutaneous manifestations in COVID-19: a first perspective. J Eur Acad
Dermatol Venereol 2020; 34:e212.
- Madigan LM,
Micheletti RG, Shinkai K. How Dermatologists Can Learn and Contribute at
the Leading Edge of the COVID-19 Global Pandemic. JAMA Dermatol 2020;
156:733.
- Suchonwanit
P, Leerunyakul K, Kositkuljorn C. Cutaneous manifestations in COVID-19:
Lessons learned from current evidence. J Am Acad Dermatol 2020; 83:e57.
- Türsen Ü,
Türsen B, Lotti T. Cutaneous sıde-effects of the potential COVID-19 drugs.
Dermatol Ther 2020; 33:e13476.
- Freeman EE,
McMahon DE, Fitzgerald ME, et al. The American Academy of Dermatology
COVID-19 registry: Crowdsourcing dermatology in the age of COVID-19. J Am
Acad Dermatol 2020; 83:509.
- Freeman EE,
McMahon DE, Lipoff JB, et al. The spectrum of COVID-19-associated
dermatologic manifestations: An international registry of 716 patients
from 31 countries. J Am Acad Dermatol 2020; 83:1118.












COMMENTS